Coordinating Ground Ambulance with Flights: A Step-by-Step Logistics Guide
- 8 hours ago
- 13 min read
On a Tuesday afternoon in October, a daughter in Phoenix watches a flight board turn red with delays, her heart sinking as she realizes her father’s medical transport team is now out of sync with the ground crew waiting in Boston. This scenario represents the primary fear for families managing long-distance medical transfers. You deserve the certainty that your loved one won't be left waiting on a cold tarmac or in a busy terminal. Successfully coordinating ground ambulance with flights requires more than just two phone calls; it demands a single point of clinical oversight to manage the 20% of domestic flights that the Bureau of Transportation Statistics reports as delayed each year.
We're here to show you how to achieve a seamless, stress-free journey through a comprehensive bedside-to-bedside solution. You'll learn how our specialized flight coordinators synchronize every movement, from the initial hospital discharge to the final clinical handoff. This guide breaks down the logistics of tarmac transfers, advanced life support integration, and the proactive communication steps that minimize transit time and protect patient dignity. By the end, you'll understand how a nurse-led approach ensures the medical handoff is handled with uncompromising precision and care.
Key Takeaways
Understand the essential "bed-to-bed" transport model, which maintains a continuous chain of medical custody for uncompromising patient safety.
Master the logistical requirements for coordinating ground ambulance with flights, from securing "Fit to Fly" clearances to verifying the necessary level of life support.
Learn how to navigate complex airport security protocols to ensure a seamless transition during both tarmac and terminal handoffs.
Discover the specialized "Standby" protocols that provide peace of mind by protecting the patient's clinical continuity during unexpected travel delays.
See why nurse-led coordination offers a superior level of medical oversight and a more compassionate experience than traditional logistics-only providers.
Table of Contents The Essentials of Coordinating Ground Ambulance with Commercial Flights Step 1: Pre-Flight Logistics and Medical Clearance Step 2: Managing the Handoff – Tarmac vs. Terminal Transfers Handling Delays and Contingency Planning The RN MEDflights Advantage: Nurse-Led Coordination
The Essentials of Coordinating Ground Ambulance with Commercial Flights
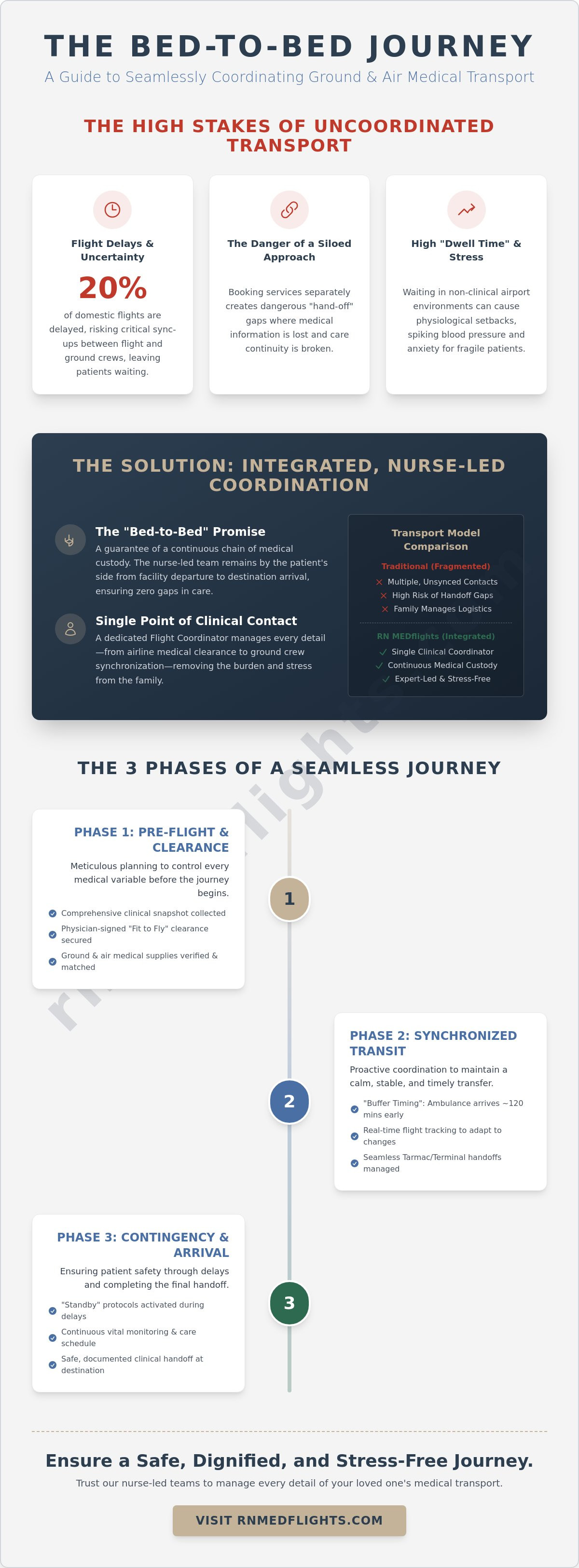
Successful medical relocation depends on a clinical standard known as Bed-to-Bed transport. This isn't merely a logistical term; it's a formal promise of a continuous chain of medical custody. From the moment a patient leaves their current facility until they're safely admitted to their destination, the medical team remains by their side. When coordinating ground ambulance with flights, synchronization becomes the most critical factor in ensuring patient safety. A gap of even thirty minutes in a drafty airport terminal can lead to physiological setbacks for a fragile patient. Within the broader context of Air medical services, the integration of ground and air assets determines the success of the mission.
Many families mistakenly adopt a siloed approach to transport. They attempt to book a local ambulance, a commercial flight, and a receiving transport separately. This creates dangerous "hand-off" points where information is lost. RN Medflights utilizes an integrated coordination approach instead. We appoint a dedicated flight coordinator as the central point of contact. This specialist manages every moving part, from verifying oxygen requirements with the airline to confirming the receiving facility is ready for the arrival. This single-source responsibility removes the burden from the family and ensures no detail is overlooked during the transition.
The Bed-to-Bed Medical Transport Philosophy
Our clinical philosophy prioritizes the minimization of "dwell time" at the airport. Dwell time refers to the period a patient spends waiting in a non-clinical environment. High-stress environments like busy terminals can spike blood pressure and increase cortisol levels. By integrating a specialized non-emergency ambulance service into the flight plan, we maintain a stable environment. This continuity of care reduces patient anxiety. It allows the medical escort to monitor vitals and administer medications on a strict schedule, just as they would in a hospital room. We treat the entire journey as a single, uninterrupted medical event.
Why Commercial Flights Require More Coordination
Commercial airlines operate on rigid schedules that don't account for medical delays. Unlike private medical jets, a commercial carrier won't hold the gate if an ambulance is delayed by traffic. This reality makes coordinating ground ambulance with flights a high-stakes task. We implement "buffer timing" strategies, often scheduling ground arrivals 120 minutes before departure to account for security protocols. Our ground crews utilize real-time flight tracking software to monitor gate changes or delays. If a flight is moved up, the ground team is notified instantly to adjust their speed or route. This vigilance ensures the patient never feels rushed, maintaining a calm and professional atmosphere throughout the transit.
Step 1: Pre-Flight Logistics and Medical Clearance
Success in coordinating ground ambulance with flights begins with meticulous clinical documentation and logistical foresight. We don't just move patients. We manage a complex continuum of care that spans hospital corridors, specialized vehicles, and aircraft cabins. This initial phase ensures every medical variable is controlled before the patient ever leaves their current facility. Our goal is to eliminate uncertainty, providing a steady hand during a high-stress transition.
The Medical Clearance Process
Our flight nurses initiate direct communication with the hospital case manager to collect a comprehensive clinical snapshot. This includes the last 12 to 24 hours of vital signs, current medication titrations, and specific oxygen requirements. It's critical to verify that the ground ambulance carries identical supplies, including backup oxygen cylinders and specific Advanced Life Support (ALS) medications, to prevent any gap in care during the transition. To meet 2026 airline safety standards, a "Fit to Fly" clearance is a formal physician-signed attestation confirming the patient can physiologically tolerate cabin pressure changes and lacks any acute contagious conditions that pose a risk to others. This document serves as the clinical foundation for the entire journey.
Logistical Data Gathering
Precision in coordinating ground ambulance with flights requires more than just a scheduled pickup time. We map out the exact entry and exit points for each airport, often selecting a Fixed Base Operator (FBO) or a specific gate that minimizes travel time on the tarmac. Our coordinators work with TSA to arrange for expedited medical screening; this ensures that life-sustaining equipment passes through security without delay. We also verify all insurance or private pay authorizations at least 48 hours before the mission to prevent administrative hurdles at the bedside. Our flight coordinators handle these details to ensure a seamless bedside-to-bedside transition for your loved one.
The final layer of safety is the "Go/No-Go" checklist, which we execute exactly 24 hours before departure. This review confirms every moving part is aligned for a successful mission:
The airline medical desk has approved all Portable Oxygen Concentrators (POCs) or ventilators for the specific flight.
The ground team is confirmed as either Basic Life Support (BLS) or ALS based on the patient's current acuity.
All weather patterns along the flight path are favorable for a stable, comfortable transport.
The receiving facility has a confirmed bed and is ready for the clinical handoff.
This methodical approach reflects our 24/7/365 commitment to integrity and patient safety. By addressing these technical details early, we reduce the emotional burden on families and provide a predictable, calm environment for the patient. We prioritize peace of mind by ensuring that the logistics are handled by experts before the first mile is traveled.
Step 2: Managing the Handoff – Tarmac vs. Terminal Transfers
The most frequent question families ask is exactly where the ambulance will meet the patient. This transition is the most complex part of coordinating ground ambulance with flights because it involves merging two different worlds: emergency medicine and aviation security. The meeting point isn't a matter of convenience; it's a decision dictated by the type of aircraft, the patient's acuity, and strict airport regulations. Our goal is to ensure the patient never feels the "gap" between the ground team and the air team.
For patients traveling on private medical jets, the transfer usually happens on the tarmac, also known as the apron. This allows the ambulance to pull directly alongside the aircraft, which minimizes the physical strain of moving the patient. However, for commercial medical escorts, security protocols usually require the handoff to occur at the terminal curb or a designated gate. Each option has specific logistical requirements:
Tarmac Transfers: These offer the highest level of privacy and speed but are typically reserved for private FBO (Fixed Base Operator) facilities.
Gate Transfers: Ideal for ambulatory patients or those using wheelchairs. This requires pre-arranged "gate passes" for the medical team.
Curb-side Transfers: The most common for commercial flights where the ground ambulance meets the flight team at a specific terminal entrance to begin the check-in process.
Understanding Tarmac Access (Apron Transfers)
Tarmac access is rarely granted for commercial flights due to TSA and FAA security mandates. If your loved one is flying commercial, the ambulance will meet our team at a pre-arranged terminal entrance. We coordinate with airport duty managers to ensure a seamless transition. For ambulatory or wheelchair-bound patients, we utilize gate-to-gate assistance. This means a flight nurse remains at the patient's side from the moment they leave the ambulance until they're safely seated on the plane.
The Clinical Handoff Protocol
The physical move is only half of the challenge. The clinical handoff is a rhythmic, disciplined process designed to prevent any lapse in care. When coordinating ground ambulance with flights, our team follows a strict 15-minute protocol during the transition. The ground paramedic provides a verbal report to the flight nurse using the SBAR (Situation, Background, Assessment, Recommendation) format. We don't just take over the stretcher; we take over the patient's entire clinical history.
During this window, the flight nurse performs several critical tasks:
Conducts an immediate assessment of vital signs to establish a baseline before takeoff.
Verifies that all medical records, imaging, and discharge summaries are physically present.
Secures and inventories patient luggage and personal belongings to prevent loss during the transition.
Ensures all medications and equipment are transferred and functioning for the duration of the flight.
This methodical approach ensures that even in a high-traffic airport environment, the patient receives the same focused attention they would in a hospital room. It's about maintaining dignity and clinical integrity throughout every foot of the journey.
Handling Delays and Contingency Planning
Families often ask what happens if a flight is delayed by two hours or more. In the high-stakes environment of coordinating ground ambulance with flights, delays aren't just a possibility; they're a variable we account for in every mission profile. We utilize a strict "Standby" protocol where ground units remain in a state of readiness, adjusted in real time based on the aircraft's transponder data. If weather or air traffic control causes a delay, our 24/7 flight coordinators manage the timing so the patient never waits on a tarmac. This level of oversight extends to "Diversion Planning." If a plane must land at an alternate airport due to unforeseen circumstances, the coordinator immediately re-routes the ground unit or activates a secondary provider at the new location to meet the aircraft the moment it lands.
The 24/7 Communication Loop
Safety requires constant visibility. We mandate real-time GPS tracking for both the air ambulance and the ground vehicle to sync their arrival within minutes. This precision prevents the patient from experiencing unnecessary exposure to the elements or long waits in a vehicle. Our team maintains a "Three-Way Call" system that connects the flight nurse, the ground crew, and the patient's family. This ensures the family knows exactly where their loved one is at every moment. Professional coordinators use a 90-minute buffer rule to ensure the ground ambulance is positioned at the airport well before the wheels touch the runway. This rhythmic coordination eliminates the stress of waiting and keeps our bedside-to-bedside promise intact.
Back-up Ground Providers
Relying on a single provider is a risk we don't take. In high-traffic hubs like New York, London, or Miami, we maintain secondary ground transport options to bypass local traffic surges or mechanical issues. Managing international logistics involves navigating different time zones and language barriers. Our nurse-led team handles these complexities by vetting providers globally to ensure they meet our uncompromising clinical standards. For families requiring movement across borders, our guide on international medical repatriation services provides deeper insight into how we maintain clinical continuity worldwide. Our 24/7/365 command center remains the steady hand that guides these moving parts, ensuring that even when plans change, the patient's care remains seamless.
If you need a logistics plan that accounts for every variable and prioritizes patient safety, contact our flight coordination team for a detailed consultation.
The RN MEDflights Advantage: Nurse-Led Coordination
Choosing a medical transport provider involves more than just booking a vehicle. It requires a deep understanding of how physiological changes at altitude affect a patient's stability. While a standard logistics coordinator manages schedules, an RN MEDflights coordinator manages lives. Our nurse-led model ensures that the person organizing the trip understands the clinical implications of every delay or detour. We specialize in coordinating ground ambulance with flights by syncing medical interventions directly with wheels-up times. This veteran-owned precision means we treat every mission with the same discipline found in military operations. Every second is accounted for, and every contingency plan is ready before the patient leaves their bed.
Our "Clinical Continuity" promise is the cornerstone of our service. Unlike other companies that hand off patients to different teams at every transition, we provide the same nurse from the initial bedside to the final destination. This eliminates the risk of information loss during handovers. Our 24/7/365 command center manages the moving parts of your trip, providing a steady hand in what is often a chaotic situation. We don't just move people; we provide a seamless medical environment that travels with them. This approach reduces the cognitive load on families who are already experiencing significant emotional distress.
Why Clinical Oversight Matters in Logistics
Medical logistics involve more than traffic patterns. They require managing medication half-lives and patient fatigue levels. Our nurses anticipate clinical needs that impact timing, such as scheduled respiratory treatments or pain management cycles. This oversight manages the emotional transfer of care for the family. You gain peace of mind knowing a single medical professional is accountable for the entire journey. We bridge the gap between hospital staff and flight crews, ensuring that dignity and safety remain the top priorities during the transition. Our staff remains vigilant, acting as a protector for the patient's health throughout the trip.
Getting Started with Your Transport
The process begins with a comprehensive initial consultation. We gather essential data, including the patient's current medical records, facility contact information, and specific equipment needs like ventilators or specialized monitors. We then build a custom itinerary tailored to your loved one’s specific health profile. Our team handles the complex task of coordinating ground ambulance with flights so you don't have to navigate the bureaucracy of airports and hospitals alone. Our 24/7/365 availability ensures we are ready to respond the moment a need arises. Contact us today for a free logistical assessment and let our experts secure the safe, professional passage your family deserves.
Ensuring Clinical Continuity for Your Loved One
Successful medical transport relies on more than just a flight. It requires a synchronized effort between clinical teams and logistics experts. From securing medical clearances to managing precise tarmac handoffs, every detail must align to prevent dangerous delays. Effectively coordinating ground ambulance with flights ensures that the patient's care never pauses during transitions. This methodical approach reduces the physical strain on families while maintaining the highest safety standards throughout the journey.
RN MEDflights brings a specialized perspective to this complex process. As a veteran-owned and nurse-operated organization with over 15 years of experience, we've built our reputation on clinical integrity. Our 24/7/365 Coordination Center provides real-time tracking of both air and ground assets to ensure every handoff is seamless. We remain dedicated to an uncompromising bedside-to-bedside standard, providing the constant medical supervision your family deserves. You don't have to navigate these logistical hurdles alone.
Request a custom bed-to-bed transport plan from RN MEDflights to begin your journey with a team that treats every patient like family. You can move forward with confidence knowing your loved one is in expert hands.
Frequently Asked Questions
How far in advance should I coordinate a ground ambulance with a flight?
You should begin coordinating ground ambulance with flights at least 48 to 72 hours before the scheduled departure. This timeframe allows our team to verify insurance coverage and secure a vehicle with the necessary clinical equipment. For international transfers, a lead time of 5 to 7 days is preferred. This extra time ensures we can navigate complex airport security permits and customs requirements without rushing the process.
Can a ground ambulance drive onto the tarmac to meet a commercial flight?
Ground ambulances cannot drive onto the tarmac for commercial flights because of strict TSA and airport security regulations. Instead, the medical team meets the ambulance at a pre-arranged terminal gate or a designated medical loading zone. Tarmac access is exclusively reserved for private air ambulance charters operating under Part 135 regulations. We manage these specific rendezvous points to ensure the patient moves efficiently through the airport infrastructure.
What happens if the flight arrives early and the ambulance isn’t there?
Our flight coordinators monitor real-time arrival data using satellite tracking software to prevent gaps in care. If a flight lands early, the patient remains under the continuous supervision of our medical escort until the vehicle arrives. We maintain 24/7/365 communication with ground dispatchers to adjust pickup times based on actual wheels-down data. This protocol ensures the patient is never left unattended in a public terminal area.
Is ground ambulance coordination included in the cost of a medical escort?
Logistical coordination for ground transport is a standard part of our bedside-to-bedside service. We manage the scheduling and clinical handoff details as part of our comprehensive care package. While the coordination service is included, the third-party ambulance providers bill their transport fees separately. We provide a detailed itinerary that outlines every leg of the journey so there are no surprises during the transition.
Do I need to call the ambulance company myself or will the escort handle it?
Our specialized flight coordinators handle all communication with ground ambulance companies so you don't have to manage complex logistics. We select providers based on their clinical capabilities and their proximity to the arrival airport. This professional oversight ensures the vehicle meets the specific medical requirements of the patient. By managing these calls, we reduce the emotional burden on the family and maintain a single point of accountability.
What medical information do I need to provide for ground transport coordination?
You must provide a current Physician’s Report, a complete medication list, and specific oxygen requirements in liters per minute. We also require the patient’s most recent 24 hour clinical vitals and mobility status, such as whether they are bed-bound or able to sit. This data allows the ground team to prepare the correct Advanced Life Support or Basic Life Support equipment before they arrive at the airport.
Can the ground ambulance transport family members along with the patient?
Most ground ambulance providers allow one family member to travel in the front passenger seat alongside the patient. This depends on the specific vehicle's weight capacity and local safety regulations. We confirm these details during the coordinating ground ambulance with flights process to ensure your family stays together. If more than one person is traveling, we recommend arranging a separate car service to meet the ambulance at the destination.
How is the handoff managed at international airports with language barriers?
We manage international handoffs by utilizing a network of multilingual dispatchers and pre-arranged GPS meeting coordinates. Our medical staff uses standardized clinical handover protocols that transcend language barriers to ensure patient safety. We also provide the ground crew with a written medical summary translated into the local language. This methodical approach maintains the integrity of care during transitions at high-traffic hubs like Heathrow or Tokyo Narita.



